Thyroid gland and blood sugar
Your thyroid gland and thyroid hormones play a major role in regulating many of your body’s biological processes, such as growth, development, and metabolism.2 Because thyroid disease interferes with metabolism, it can alter your blood sugar. This increases your risk of developing diabetes, and it makes it harder to manage your blood sugar if you already have diabetes.
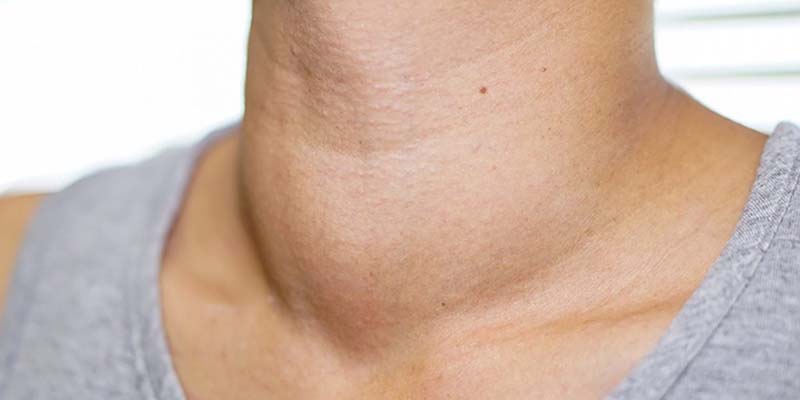
Hyperthyroidism, which is overactive thyroid hormone, and hypothyroidism, which is underactive thyroid hormone, are both associated with mild hyperglycemia (elevated glucose levels).The thyroid, a small, butterfly-shaped gland that wraps around your windpipe, has a highly important job. As the largest gland in the endocrine system, it regulates hormones and ensures growth, metabolism and development all occur at “normal” rates. It is believed that the chronically high blood sugar that can be induced by thyroid disease may contribute to the development of metabolic syndrome, a pre-diabetic state. Untreated metabolic syndrome can progress to type 2 diabetes
The importance of the thyroid gland
Hyperthyroidism is caused by the thyroid gland producing too much thyroid hormone. It may be caused by Graves disease (an autoimmune disease in which the body’s own cells attack the thyroid gland), one or more thyroid nodules, ingesting too much iodine, inflammation of the thyroid gland or taking too much thyroid medication. Symptoms include:
- Sweating
- Weight loss
- Diarrhea
- Distraction
- Menstrual changes in women
- Rapid heart rate
- Thick skin on the knees, elbows, and shins
Thyroid Hormone Effects on Diabetes
Diabetes is a chronic disease in which the body cannot use or store glucose. Glucose is a type of sugar that, if it accumulates in the blood, causes high blood sugar.
The effect on carbohydrate metabolism can potentially lead to disruptions in diabetes control. Additionally, excessive thyroid hormones increase the rate of digestive tract absorption and thyroid hormone levels and therefore increase insulin resistance and insulin degradation. In hyperthyroidism, glycogen synthesis and degradation increase, leading to decreased glycogen levels.
Additionally, in patients with undetected diabetes, hyperthyroidism can unmask diabetes because glucose levels can be abnormally elevated because of increased insulin resistance.3 Increased dosages of diabetes medications may be necessary in those already treated, until thyroid function is stabilized and resultant glucose stabilization occurs.
Thyroid Disease and Insulin
Diabetes can cause alterations in thyroid hormone levels. Insulin imitates the actions of thyroid hormones in some tissues of the body, which decreases the production of thyroid hormones. But insulin also functions in the opposite way thyroid hormones do in other tissues, which increases thyroid hormone levels. Excess or deficient insulin can induce changes in thyroid hormone production and activity. Looking at the association from another direction, the metabolic changes of thyroid disease can interfere with the effects of insulin, whether endogenous (produced by your body) or taken as a medical treatment for diabetes.
Hyperthyroidism increases metabolism and can cause insulin to be processed and eliminated from the body more quickly than normal.5 Some people with type 1 diabetes who are also diagnosed with hyperthyroidism may need to take higher doses of insulin until thyroid hormones are stabilized.
How Hyperthyroidism May Affect Diabetic Patients
The presence of thyroid dysfunction may affect diabetes control. Hyperthyroidism is typically associated with worsening glycemic control and increased insulin requirements. There is underlying increased hepatic gluconeogenesis, rapid gastrointestinal glucose absorption, and probably increased insulin resistance. Indeed, thyrotoxicosis may unmask latent diabetes.
In practice, there are several implications for patients with both diabetes and hyperthyroidism.
- First, in hyperthyroid patients, the diagnosis of glucose intolerance needs to be considered cautiously, since the hyperglycemia may improve with treatment of thyrotoxicosis.
- Second, underlying hyperthyroidism should be considered in diabetic patients with unexplained worsening hyperglycemia.
- Third, in diabetic patients with hyperthyroidism, physicians need to anticipate possible deterioration in glycemic control and adjust treatment accordingly. Restoration of euthyroidism will lower blood glucose level.
Because hyperthyroidism can cause serious adverse effects on glycemic control and possibly worsen pre-existing coronary artery disease, it is desirable to consider definitive treatment with radioactive iodine therapy whenever possible. There is no contraindication to the use of antithyroid medications in diabetic patients.
References
https://spectrum.diabetesjournals.org/content/19/3/148
https://www.verywellhealth.com/thyroid-disease-and-diabetes-3289616
http://journal.diabetes.org/clinicaldiabetes/v18n12000/pg38.htm
https://www.boostthyroid.com/blog/2019/5/17/diabetes-hashimotos-and-an-underactive-thyroid