What is thyroiditis?
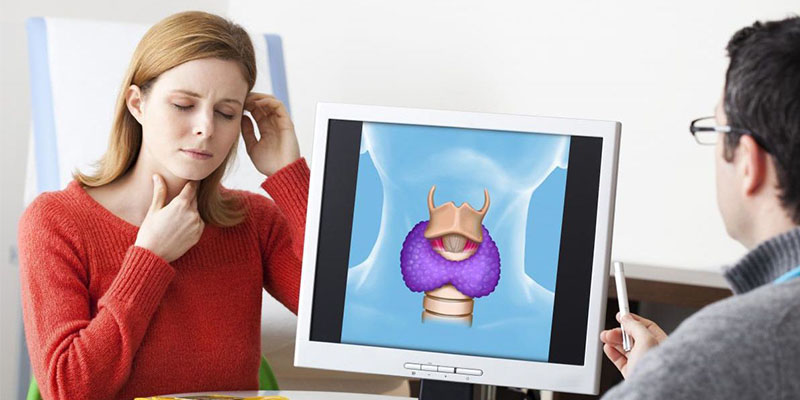
Thyroiditis refers to a group of disorders that cause inflammation of the thyroid. Your thyroid is the gland located in the front of your neck below your Adam’s apple. The thyroid makes hormones that control your metabolism and affect how your body works. Metabolism is how your body processes substances to produce energy, or burn calories.
Types of thyroiditis
There are several types of thyroiditis:
- Hashimoto’s thyroiditis
- Acute thyroiditis
- Silent thyroiditis
- Postpartum thyroiditis
- Thyroiditis caused by radiation therapy
- Drug-induced thyroiditis
How to diagnose thyroiditis
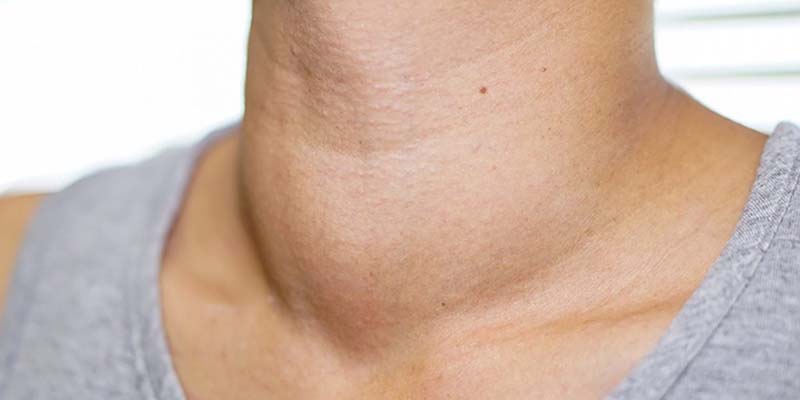
Examination and examination of clinical signs: Your doctor will feel and examine your neck to see if the thyroid gland is enlarged or inflamed. They’ll also ask you about your symptoms and your recent medical history.
Thyroid stimulating hormone test: Thyroid function tests measure the amounts of hormones (thyroid-stimulating hormone or TSH, T3, and T4) in the blood. TSH comes from the pituitary gland and stimulates the thyroid gland to produce T4 and T3. The thyroid gland produces the hormones T4 and T3 that exert the action of thyroid hormone in the body. T3 and T4 are called thyroid hormones. When you are hypothyroid, you have higher TSH levels because your body is trying to tell your thyroid to make more hormones. The reverse is true with hyperthyroidism: TSH levels are below normal and thyroid hormone levels are high.
Thyroid antibody tests: measure thyroid antibodies that include antithyroid (microsomal) antibodies (TPO) or thyroid receptor stimulating antibodies (TRAb).
Erythrocyte sedimentation rate (ESR or sed rate) indicates inflammation by measuring how fast red blood cells fall. The ESR is high in sub-acute thyroiditis.
Thyroid scans using radioactive iodine: The thyroid is the only location in the body that takes. During this scan a small amount of radioactive iodine is swallowed or a similar material, 99m-technetium, is injected into the blood, and then an imaging study of the thyroid is taken that reveals localization of the radioactivity. Increased uptake of the radioactive material in the thyroid gland indicates hyperthyroidism, while decreased uptake is present in hypothyroidism.
Biopsy: Fine needle aspiration and biopsy are techniques that remove a sample of cells or tissue from the thyroid gland for examination and diagnosis by a pathologist, who is a physician trained in the diagnosis of conditions based on tissue samples. Fine needle aspiration (FNA) uses a long, thin needle to withdraw a sample of cells from the thyroid. FNA can be performed in the doctor’s office.
Ultrasound: sonogram of the thyroid, is used very frequently to evaluate the anatomy of the thyroid gland. It can show a nodule (a growth) in the thyroid gland, a change in blood flow (Doppler mode) and echo texture (intensity/density) of the gland.
How to treat thyroiditis
Hashimoto’s Thyroiditis
Hashimoto’s thyroiditis, also called autoimmune or chronic lymphocytic thyroiditis, is the most common type of thyroiditis. Hashimoto’s thyroiditis is the most common cause of hypothyroidism. The thyroid gland is always enlarged in Hashimoto’s thyroiditis. The radioactive iodine uptake may be paradoxically high. As the disease progresses, the TSH (thyroid stimulating hormone) increases since the pituitary is trying to induce the thyroid to make more hormone, the T4 (a different thyroid hormone) falls since the thyroid can’t make it, and the patient becomes hypothyroid. This sequence of events can occur over a relatively short span of a few weeks or may take several years. Treatment should begin with thyroid hormone replacement. This prevents or corrects the hypothyroidism, and it also generally keeps the gland from getting larger.In most cases, the thyroid gland will decrease in size once thyroid hormone replacement is started.Thyroid antibodies are present in 95% of patients with Hashimoto’s thyroiditis and serve as a useful “marker” in identifying the disease without thyroid biopsy or surgery.
De Quervain’s Thyroiditis
De Quervain’s thyroiditis (also called subacute or granulomatous thyroiditis) was first described in 1904 and is much less common than Hashimoto’s thyroiditis. The thyroid gland generally swells rapidly and is very painful and tender. The gland discharges thyroid hormone into the blood and the patients become hyperthyroid; however, the gland quits taking up iodine (radioactive iodine uptake is very low), and the hyperthyroidism generally resolves over the next several weeks. Thyroid antibodies are not present in the blood, but the sedimentation rate (which measures inflammation) is very high. Possible medications include:
- Over-the-counter nonsteroidal anti-inflammatory
- Corticosteroids
- Beta-blockers
Nearly all patients recover, and the thyroid gland returns to normal after several weeks or months.A few patients will become hypothyroid once the inflammation settles down and therefore will need to stay on thyroid hormone replacement indefinitely.
Silent Thyroiditis
Silent thyroiditis is the third and least common type of thyroiditis. It was treated as Graves’ disease before that. This type of thyroiditis resembles a combination of Hashimoto’s thyroiditis and De Quervain’s thyroiditis. The blood thyroid test is high and the radioactive iodine uptake is low (like De Quervain’s thyroiditis). The disease usually needs no treatment, and 80% of patients show complete recovery and return of the thyroid gland to normal after 3 months. Symptoms are similar to Graves’ disease except milder. Treatment is usually bed rest with beta blockers to control palpitations (drugs to prevent rapid heart rates).
Reference
https://www.webmd.com/women/understanding-thyroid-problems-treatment#4
https://www.healthline.com/health/subacute-thyroiditis#subtypes
https://familydoctor.org/condition/thyroiditis/
https://my.clevelandclinic.org/health/diseases/15455-thyroiditis/management-and-treatment
https://www.endocrineweb.com/conditions/thyroid/thyroiditis