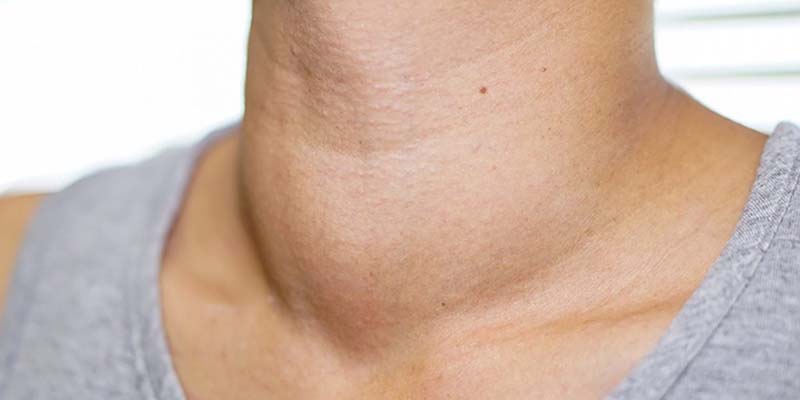
Hyperthyroidism
HORMONE CHANGES. A normal pregnancy results in a number of important physiological and hormonal changes that alter thyroid function. These changes mean that laboratory tests of thyroid function must be interpreted with caution during pregnancy. Pregnant women with hyperthyroidism need careful management as some may be at increased risk of fetal loss, pre-eclampsia, heart failure, premature labour, and having a low birthweight baby
What are the normal changes in thyroid function associated with pregnancy?
Thyroid function tests change during pregnancy due to the influence of two main hormones: human chorionic gonadotropin (hCG), the hormone that is measured in the pregnancy test and estrogen, the main female hormone. HCG can weakly turn on the thyroid and the high circulating hCG levels in the first trimester may result in a slightly low TSH. When this occurs, the TSH will be slightly decreased in the first trimester and then return to normal throughout the duration of pregnancy. Estrogen increases the amount of thyroid hormone binding proteins in the serum which increases the total thyroid hormone levels in the blood since >99% of the thyroid hormones in the blood are bound to these proteins. However, measurements of “Free” hormone (that are not bound to protein, representing the active form of the hormone) usually remain normal. The thyroid is functioning normally if the TSH and Free T4 remain in the trimester-specific normal ranges throughout pregnancy.
SIZE CHANGES. The thyroid gland can increase in size during pregnancy (enlarged thyroid = goiter). However, pregnancy-associated goiters occur much more frequently in iodine-deficient areas of the world. It is relatively uncommon in the United States. If very sensitive imaging techniques (ultrasound) are used, it is possible to detect an increase in thyroid volume in some women. This is usually only a 10-15% increase in size and is not typically apparent on physical examination by the physician. However, sometimes a significant goiter may develop and prompt the doctor to measure tests of thyroid function.
What are the most common causes of hyperthyroidism during pregnancy?
Overall, the most common cause of hyperthyroidism in women of childbearing age is Graves’ disease, which occurs in 0.2% of pregnant patients. In addition to other usual causes of hyperthyroidism, very high levels of hCG, seen in severe forms of morning sickness (hyperemesis gravidarum), may cause transient hyperthyroidism in early pregnancy. The correct diagnosis is based on a careful review of history, physical exam and laboratory testing.
what are the risks of graves disease to the mothers?
Graves’ disease may present initially during the first trimester or may be exacerbated during this time in a woman known to have the disorder. In addition to the classic symptoms associated with hyperthyroidism, inadequately treated maternal hyperthyroidism can result in early labor and a serious complication known as pre-eclampsia. Additionally, women with active Graves’ disease during pregnancy are at higher risk of developing very severe hyperthyroidism known as thyroid storm. Graves’ disease often improves during the third trimester of pregnancy and may worsen during the post partum period.
What are the risks of hyperthyroidism in pregnancy?
Pre-eclampsia, heart failure, fetal loss, premature labour, and having a low birthweight baby are more likely to occur in untreated or poorly controlled thyrotoxic women than in those receiving adequate treatment. A retrospective review of 11 reports documented a 5.6% incidence of fetal death or stillbirth in 249 pregnancies and a further 5% incidence of fetal and neonatal abnormalities. Preterm delivery, perinatal mortality, and maternal heart failure were more common in women who remained thyrotoxic despite treatment or whose hyperthyroidism was first diagnosed during pregnancy.
Women with thyroid hormone resistance (where thyroid hormone and thyrotrophin concentrations are inappropriately high—that is, not due to autoimmunity) also have a high miscarriage rate, indicating a direct toxic effect of thyroid hormones on the fetus.
References
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2270981/
https://www.ijrcog.org/index.php/ijrcog/article/viewFile/486/457/