papillary thyroid cancer
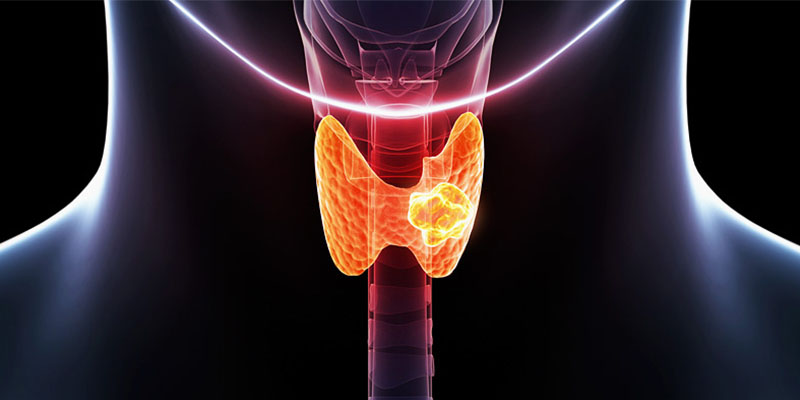
Papillary thyroid carcinoma is the most common thyroid cancer. About 80% of all thyroid cancers cases are papillary thyroid cancer. You may have even heard your doctor talk about metastatic papillary thyroid cancer (“metastatic” means that it has spread beyond your thyroid gland). In the absence of timely diagnosis and treatment, Cervical metastasis spread to lymph nodes in the neck. Most commonly, papillary thyroid cancers are totally asymptomatic. However, the most common symptom is a mass in the neck. Papillary carcinoma typically arises as a solid, irregular or cystic mass that comes from otherwise normal thyroid tissue. Here’s a look at the symptoms, diagnosis, and treatment options for papillary thyroid cancer.
Methods for diagnosis of papillary thyroid cancer
Doctors and specialists perform various tests on the patient to determine the type of tumor and the stage of cancer. These include:
- Ultrasound of the neck and thyroid gland
- CT Scan
- Color Imaging (MRI)
- blood test
- Laryngoscopy (examination of vocal cords)
- Biopsy
Symptoms of Papillary Thyroid Cancer
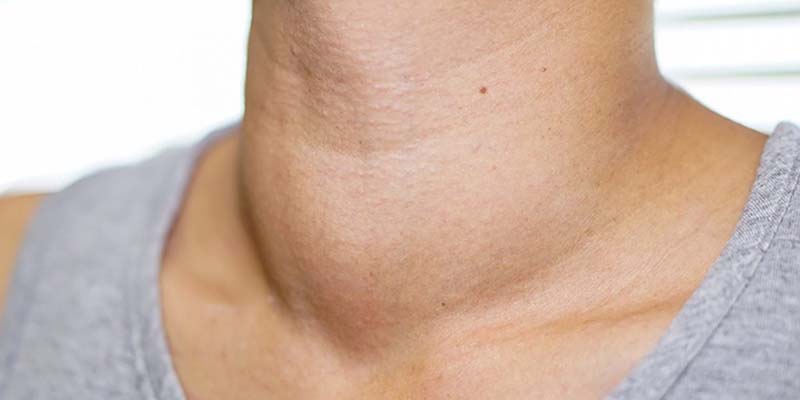
Often, you won’t have any. You might only find out about it because of an imaging test for another problem. Or, during a routine physical, your doctor might just happen to feel a lump, called a nodule, on your thyroid. Nodules are growths that may be solid or filled with fluid. As a nodule gets bigger, you may start to have symptoms like:
- Hard time swallowing
- Sore throat or hoarseness that doesn’t go away
- Swollen lymph nodes in your neck
- Trouble breathing, especially when you lie down
Strategies for the treatment of papillary thyroid cancer
There are three main parts to the treatment of papillary thyroid cancer:
Surgery: The best treatment for papillary thyroid cancer is almost always total thyroidectomy (i.e. removal of the entire thyroid). There are a few very specific situations in which some doctors will remove only the half of the thyroid with the cancer (i.e. thyroid lobectomy), but most doctors recommend a total thyroidectomy because:Most papillary thyroid cancers are multifocal (i.e. in more than one part of the thyroid). The recurrence rate (i.e. chance that cancer comes back) is lower in patients who have had a total thyroidectomy than a lobectomy. If the lateral neck lymph nodes (i.e. the lymph nodes surrounding the carotid artery and jugular vein) are involved with papillary thyroid cancer, then an operation called a modified radical neck dissection will be performed either at the time of the total thyroidectomy. This operation involves removing the lymph nodes along one side of the neck.
Thyroid Hormone Suppression: After removal of the entire thyroid, patients will need to take thyroid hormone replacement pills (usually one pill a day for the rest of their lives) in order to replace the hormone that the thyroid would normally make. Patients with thyroid cancer are typically given a slightly higher dose than patients without thyroid cancer in order to suppress or block any stimulation for thyroid cancer cells to grow. The thyroid hormone replacement pill tricks the brain into thinking that enough thyroid hormone is being manufactured by the thyroid gland, therefore shutting down the brain’s production of TSH (thyroid stimulating hormone which normally encourages the thyroid to make thyroid hormone). This is important because if TSH is left at high levels, it can stimulate both the remaining normal thyroid as well as any thyroid cancer and metastases to grow and enlarge.
Radioactive Iodine (RAI) Ablation: Depending on the final pathology, the patient may need RAI ablation or what some doctors call remnant ablation. RAI ablation is not like the traditional external beam radiation which can be difficult on patients. RAI ablation is a pill that is taken once and usually causes few side effects. In this therapy, radioactive iodine is given to destroy any remaining thyroid cells (both cancer and benign) after total thyroidectomy. RAI ablation does not improve the overall excellent prognosis, but rather, it decreases the recurrence rate (i.e. chance of cancer coming back).
Follow-up
After surgery for papillary thyroid cancer, it is important to be examined regularly for signs that the cancer may have recurred. In general, patients should have a thyroglobulin blood test, TSH level, and USG of the neck every 6 months to a year.
Recurrence of Thyroid Cancer
Although thyroid cancer recurrence is not common, there are many treatment options available if it happens. If a cancer recurrence is detected in the neck lymph nodes, the best course of action is usually an operation to remove the affected node(s) or additional treatment with RAI ablation.
Reference
https://columbiasurgery.org/conditions-and-treatments/papillary-thyroid-cancer
https://www.endocrineweb.com/conditions/thyroid-cancer/papillary-cancer
https://www.webmd.com/cancer/papillary-thyroid-carcinoma-about#3