Hashimoto
Hypothyroidism, or an underactive thyroid, is a common problem. the most common cause of hypothyroidism is Hashimoto’s thyroiditis. Hypothyroidism is treated by thyroid hormone and returning thyroid hormone levels to the normal range usually resolves symptoms in most patients. However, in some patients, symptoms may persist despite what appears to be adequate treatment based on blood tests of thyroid function. This raises the possibility that some symptoms may be related to the autoimmune condition itself
What is Hashimoto’s Thyroid?
Hashimoto’s thyroiditis is an autoimmune condition where your immune system attacks healthy thyroid cells. Indeed Hashimoto’s thyroiditis is an autoimmune disorder where antibodies attack the thyroid, causing inflammation and destruction of the gland. Characteristic of Hashimoto’s thyroiditis are high antibodies to thyroid peroxidase (TPO Ab) on blood tests. Some studies suggest that TPOAb may cross-react with tissues other than the thyroid and may contribute to inflammation and general symptoms. Indeed, some patients with high TPOAb levels and normal thyroid hormone levels (without medication) will present with symptoms similar to those of patients with hypothyroidism. If persistent symptoms in patients with Hashimoto’s thyroiditis are caused by the active autoimmune process rather than by thyroid hormone status, removing the thyroid gland through surgery may reduce the levels of the TPOAb and improve some symptoms.
What Are the Symptoms (and Causes) of a Hashimoto’s Flare-Up?
Hashimoto’s thyroiditis is an autoimmune condition where your immune system attacks healthy thyroid cells.
When Hashimoto’s thyroiditis flares up, you may begin to feel some of the symptoms of hypothyroidism. These can include things like:
- fatigue
- aches and pains in your muscles and joints
- constipation
- unexplained weight gain
- skin that’s pale and dry
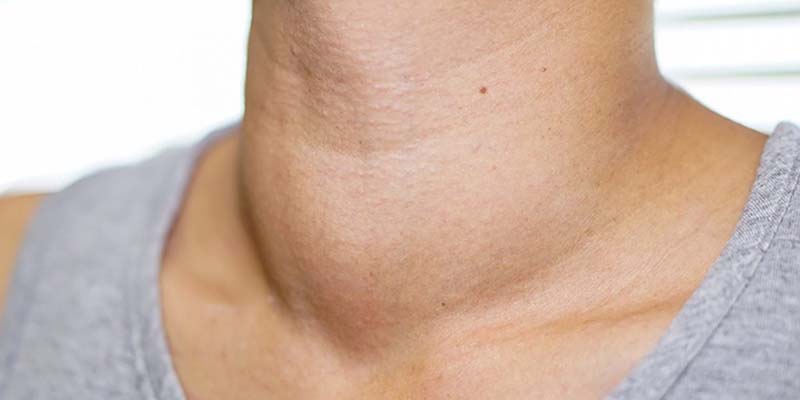
- enlarged thyroid (goiter)
- sensitivity to cold
- hair that’s dry or brittle
- hair loss
- brittle nails
- muscle weakness
- slow heart rate (bradycardia)
- problems with memory
- depression
- irregular or heavy menstrual periods
The conventional treatment for hypothyroidism, including Hashimoto’s thyroiditis, is to use a medication called levothyroxine to replace the missing thyroid hormone. Levothyroxine is a synthetic version of thyroid hormone.
Sometimes factors like stress and other medications can affect the function of your thyroid or of your levothyroxine absorption. This can cause your hypothyroidism symptoms to flare up.
What is the treatment for Hashimoto’s Thyroiditis?
- Thyroid Hormone Replacement
Hashimoto’s thyroiditis that causes hypothyroidism is treated with a medication called levothyroxine. This is a synthetic version of thyroid hormone that helps replace the hormones that your thyroid isn’t producing.
The proper dose of levothyroxine is different for everyone. If you’re taking the correct dose of levothyroxine, you shouldn’t experience a flare-up.
Since a variety of factors can impact your thyroid as well as the effectiveness of levothyroxine, it’s important to have your thyroid levels checked regularly. These factors include:
- diet
- medications
- stress
You should have your thyroid levels checked once or twice per year.
- Anti-inflammatory approaches
When the inflammatory condition is very severe, some doctors consider a short duration of steroid therapy. Alternative medical approaches such as gluten free and avoidance of food coloring in exacerbation of Hashimoto’s disease has been advocated as well.
- Thyroid Surgery
Thyroid Surgery may play a role in the management of patients with Hashimoto’s thyroiditis:
When is Hashimoto’s thyroid surgery recommended?
- symptomatic thyroiditis
- thyroid enlargement and producing symptoms from its size
- mood or hormonal dysfunction.
- A thyroid nodule is present and an FNA is suspicious for thyroid cancer
- The inflammatory condition has exhausted medical management and causing tenderness and pain in the neck or referred pain to the surrounding area. This is a rare event.
Hashimoto’s thyroiditis surgery should only be performed by highly expert thyroid surgeons. An occasional thyroid surgeon should not do this surgery.
Lifelong thyroid hormone replacement medication is almost certainly needed after thyroid surgery when Hashimoto’s disease is present.
References
https://www.thyroidcancer.com/hashimotos-thyroiditis
https://www.thyroid.org/patient-thyroid-information/ct-for-patients/july-2019/vol-12-issue-7-p-8-9/
https://www.healthline.com/health/symptoms-of-hashimotos-flare-up#symptoms